Resources
A list of resources for prescribers and references to evidence
Different types of resources provided across the Antibiotic Optimisation website are listed below.
More information about how and why to use the three promoted strategies to optimise antibiotic use can be found on the main pages for prescribers:
Support materials available on this website which can be printed on A4:
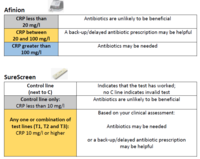
Instructions for using the Afinion CRP tests (pdf)
Read more on discussing leaflets interactively in consultations. You can download the leaflets below:
|
Treating Your Infection - RTI leaflet (A4 format) 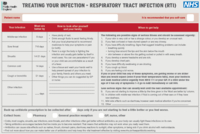
|
Treating Your Infection - UTI leaflet (A4 format) 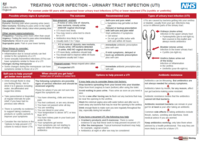
|
|
When should I worry? booklet (A6 booklet format) 
|
Caring for Coughs booklet (A6 booklet format) 
|
|
Bronchitis and cough infosheet (A4 format)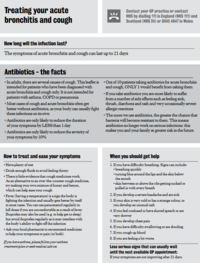 
|
Cold or upper RTI infosheet (A4 format) 
|
|
Sinusitis infosheet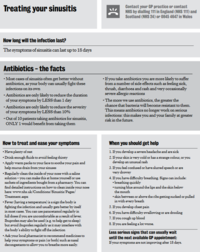 
|
Sore throat infosheet 
|
|
Child with bronchitis and cough infosheet (A4 format) 
|
Child with otitis media infosheet (A4 format) 
|
Here are some other resources helpful for optimising antibiotic prescribing:
- TARGET Antibiotic Toolkit - 'Treat Antibiotics Responsibly, Guidance, Education, Tools' - a set of resources for primary care teams to promote prudent antibiotic prescribing. The resources include patient leaflets, resources for clinical and waiting areas, audit toolkits, self-assessment checklists and action plans; training resources (such as webinars).
- TARGET Antibiotics - Prescribing in Primary Care - FutureLearn free online course for primary care professionals to target the use of antibiotics to reduce antimicrobial resistance.
- STAR online training - 'Stemming the Tide of Antibiotic Resistance' - an online training on practical techniques for improving consultations for common infections; provided as part of Clinical Professional Development.
- Antimicrobial Stewardship: Managing Antibiotic Resistance - an online training course to promote safe, high-quality antibiotic use; provided through the Future Learn platform.
- RCGP 'Antibiotic resistance in Primary Care' e-module (note: to access the training you need to be registered with RCGP).
- 'Reducing Antimicrobial Resistance: An Introduction' by Health Education England.
The following websites provide data on antibiotic prescribing rates in general practices and CCGs, and show how they compare locally and nationally:
- Fingertips - Practice and CCG-level prescribing data, published quarterly and compared nationally.
(For practice-level data, follow the link, then in the top bar select 'Antibiotic Prescribing'; in Area Type select ‘GP’; in Areas Grouped By select ‘CCGs (2018/19)’; in ‘CCGs (2018/19)’ select your CCG. Your practice will be listed in the data table below.)
- OpenPrescribing - Practice and CCG-level prescribing data, published monthly (with a longitudinal trend); compared to other practices within the same CCG.
(For practice-level data, use the link, select your practice, then select 'Antimicrobial Stewardship' measures.)
- NHS England Dashboard - CCG-level data related to antibiotic prescribing and related quality targets; the NHS England Antibiotic Quality Premium Monitoring Dashboard is produced by the NHS Business Services Authority to support NHS England in monitoring CCG performance in the delivery of the Antibiotic Quality Premium.
References
- Little P, Stuart B, Francis N, Douglas E, Tonkin-Crine S, Anthierens S, Cals JW, Melbye H, Santer M, Moore M, Coenen S, Butler C … Yardley L. Effects of internet-based training on antibiotic prescribing rates for acute respiratory-tract infections: a multinational, cluster, randomised, factorial, controlled trial. The Lancet. 2013; 382(9899):1175-82. https://doi.org/10.1016/S0140-6736(13)60994-0
- Francis NA, Butler CC, Hood K, Simpson S, Wood F, Nuttall J. Effect of using an interactive booklet about childhood respiratory tract infections in primary care consultations on reconsulting and antibiotic prescribing: a cluster randomised controlled trial. BMJ. 2009; 339:b2885. https://doi.org/10.1136/bmj.b2885
- Costelloe C, Lovering A, Hay AD. Effect of antibiotic prescribing in primary care on antimicrobial resistance in individual patients: systematic review and meta-analysis. BMJ. 2010; 340:c2096. https://doi.org/10.1136/bmj.c2096
- Bakhit M, Hoffmann T, Scott AM, Beller E, Rathbone J, Del Mar C. Resistance decay in individuals after antibiotic exposure in primary care: a systematic review and meta-analysis. BMC Medicine. 2018;16(1):126. https://doi.org/10.1186/s12916-018-1109-4
- Van Hecke O, Fuller A, Bankhead C, Jenkins-Jones S, Francis N, Moore M, Butler C, Wang K. British Journal of General Practice. 2019; 69:686. https://doi.org/10.3399/bjgp19X705089
- Cabral C, Ingram JC, Hay AD, Horwood JP. “They just say everything's a virus” - parent's judgment of the credibility of clinician communication in primary care consultations for respiratory tract infections in children: A qualitative study. Patient Education and Counseling. 2014; 95:248-253. https://doi.org/10.1016/j.pec.2014.01.010
- Mustafa M, Wood F, Butler CC, Elwyn G. Managing expectations of antibiotics for upper respiratory tract infections: a qualitative study. The Annals of Family Medicine. 2014;12(1):29-36. http://www.annfammed.org/content/12/1/29
- Heritage J, Elliott MN, Stivers T, Richardson A, Mangione-Smith R. Reducing inappropriate antibiotics prescribing: the role of online commentary on physical examination findings. Patient Education and Counseling. 2010;81(1):119-25. https://doi.org/10.1016/j.pec.2009.12.005
- Mangione-Smith R, McGlynn EA, Elliott MN, Krogstad P, Brook RH. The relationship between perceived parental expectations and pediatrician antimicrobial prescribing behavior. Pediatrics. 1999;103(4 Pt 1): 711–718. https://doi.org/10.1542/peds.103.4.711
- Butler CC, Rollnick S, Pill R, Maggs-Rapport F, Stott N. Understanding the culture of prescribing: qualitative study of general practitioners' and patients' perceptions of antibiotics for sore throats. BMJ. 1998;317(7159):637-42. https://doi.org/10.1136/bmj.317.7159.637
- Thompson M, Vodicka TA, Blair PS, Buckley DI, Heneghan C, Hay AD. Duration of symptoms of respiratory tract infections in children: systematic review. BMJ. 2013;347. https://www.bmj.com/content/347/bmj.f7027
- Little P, Williamson I, Warner G, Gould C, Gantley M, Kinmonth A. Open randomised trial of prescribing strategies in managing sore throat. BMJ. 1997;314(7082):722. https://www.bmj.com/content/314/7082/722
- Williamson IG, Rumsby K, Benge S, et al. Antibiotics and topical nasal steroid for treatment of acute maxillary sinusitis: a randomized controlled trial. JAMA. 2007;298(21):2487-2496. https://jamanetwork.com/journals/jama/fullarticle/209649
- Little P, Rumsby K, Kelly J, Watson L, Moore M, Warner G, Fahey T, Williamson I. Information leaflet and antibiotic prescribing strategies for acute lower respiratory tract infection: a randomized controlled trial. JAMA. 2005; 22;293(24):3029-35. https://jamanetwork.com/journals/jama/article-abstract/201123
- Little P, Stuart B, Moore M, Coenen S, Butler CC, Godycki-Cwirko M, Mierzecki A, Chlabicz S, Torres A, Almirall J, Davies M. Amoxicillin for acute lower-respiratory-tract infection in primary care when pneumonia is not suspected: a 12-country, randomised, placebo-controlled trial. The Lancet Infectious Diseases. 2013;13(2):123-9. https://doi.org/10.1016/S1473-3099(12)70300-6
- Side effects ‘1 in 10 people’ - British National Formulary: Phenoxymethylpenicillin. Available on: https://bnf.nice.org.uk/drug/phenoxymethylpenicillin.html#sideEffects
- Butler CC, Simpson SA, Dunstan F, Rollnick S, Cohen D, Gillespie D, Evans MR, Alam MF, Bekkers MJ, Evans J, Moore L. Effectiveness of multifaceted educational programme to reduce antibiotic dispensing in primary care: practice based randomised controlled trial. BMJ. 2012; 344:d8173. https://doi.org/10.1136/bmj.d8173
- Köchling A, Löffler C, Reinsch S, Hornung A, Böhmer F, Altiner A, Chenot JF. Reduction of antibiotic prescriptions for acute respiratory tract infections in primary care: a systematic review. Implementation Science. 2018;13(1):47. https://implementationscience.biomedcentral.com/articles/10.1186/s13012-018-0732-y
- Tonkin-Crine SK, San Tan P, van Hecke O, Wang K, Roberts NW, McCullough A, Hansen MP, Butler CC, Del Mar CB. Clinician‐targeted interventions to influence antibiotic prescribing behaviour for acute respiratory infections in primary care: an overview of systematic reviews. Cochrane Database of Systematic Reviews. 2017(9). https://doi.org/10.1002/14651858.CD012252.pub2
- O'Sullivan JW, Harvey RT, Glasziou PP, McCullough A. Written information for patients (or parents of child patients) to reduce the use of antibiotics for acute upper respiratory tract infections in primary care. Cochrane Database of Systematic Reviews. 2016(11). https://doi.org/10.1002/14651858.CD011360.pub2
- Macfarlane J, van Weel C, Holmes W, Gard P, Thornhill D, Macfarlane R, Hubbard R. Reducing antibiotic use for acute bronchitis in primary care: blinded, randomised controlled trial of patient information leaflet. BMJ. 2002; 324(7329):91-4. https://www.bmj.com/content/324/7329/91.1
- Bunten AK, Hawking MKD, McNulty CAM. Patient information can improve appropriate antibiotic prescribing. Nursing In Practice. 2015; 82:61-3. https://www.nursinginpractice.com/patient-information-can-improve-appropriate-antibiotic-prescribing
- Gulliford MC, Prevost AT, Charlton J, Juszczyk D, Soames J, McDermott L, Sultana K, Wright M, Fox R, Hay AD, Little P. Effectiveness and safety of electronically delivered prescribing feedback and decision support on antibiotic use for respiratory illness in primary care: REDUCE cluster randomised trial. BMJ. 2019; 13;364:l236. https://doi.org/10.1136/bmj.l236
- NICE Clinical Guidelines [CG191] Pneumonia in adults: diagnosis and management. 2014. https://www.nice.org.uk/guidance/cg191
- NICE Medtech innovation briefing [MIB81] Alere Afinion CRP for C-reactive protein testing in primary care. 2016. https://www.nice.org.uk/advice/mib81
- Aabenhus R, Jensen JU, Jørgensen KJ, Hróbjartsson A, Bjerrum L. Biomarkers as point‐of‐care tests to guide prescription of antibiotics in patients with acute respiratory infections in primary care. Cochrane Database of Systematic Reviews. 2014(11). https://doi.org/10.1002/14651858.CD010130.pub2
- Cals JWL, Butler CC, Hopstaken RM, Hood K, Dinant G. Effect of point of care testing for C reactive protein and training in communication skills on antibiotic use in lower respiratory tract infections: cluster randomised trial. BMJ. 2009; 338:b1374. https://doi.org/10.1136/bmj.b1374
- Butler CC, Gillespie D, White P, Bates J, Lowe R, Thomas-Jones E, Wootton M, Hood K, Phillips R, Melbye H, Llor C. C-Reactive Protein Testing to Guide Antibiotic Prescribing for COPD Exacerbations. New England Journal of Medicine. 2019; 381(2):111-20. https://doi.org/10.1056/NEJMoa1803185
- Little P, Moore M, Kelly J, Williamson I, Leydon G, McDermott L, ... Stuart B. Delayed antibiotic prescribing strategies for respiratory tract infections in primary care: pragmatic, factorial, randomised controlled trial. BMJ. 2014; 348:g1606. https://doi.org/10.1136/bmj.g1606
- Little P, Stuart B, Hobbs FR, Butler CC, Hay AD, Delaney B, ... Everitt H. Antibiotic prescription strategies for acute sore throat: a prospective observational cohort study. The Lancet Infectious Diseases. 2014; 14(3):213-219. https://doi.org/10.1016/S1473-3099(13)70294-9
- Little P, Stuart B, Smith S, Thompson MJ, Knox K, van den Bruel A, ... Mant D. Antibiotic prescription strategies and adverse outcome for uncomplicated lower respiratory tract infections: prospective cough complication cohort (3C) study. BMJ. 2017; 357:j2148. https://doi.org/10.1136/bmj.j2148
- Spurling GK, Del Mar CB, Dooley L, Foxlee R, Farley R. Delayed antibiotic prescriptions for respiratory infections. Cochrane Database of Systematic Reviews. 2017(9). https://doi.org/10.1002/14651858.CD004417.pub5